高血圧
Hypertension/ja
| 高血圧 | |
|---|---|
| Other names | Arterial hypertension, high blood pressure |
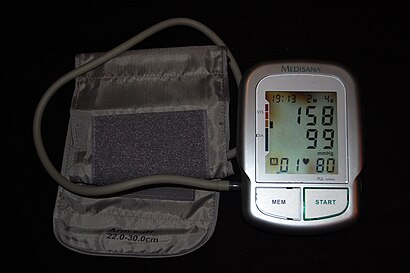 | |
| 自動化された腕の血圧計で動脈高血圧(収縮期血圧で示される。158 mmHg、拡張期血圧は99 mmHg、心拍数は80拍/分である) | |
| Specialty | 循環器学 |
| Symptoms | None |
| Complications | Coronary artery disease/ja, stroke/ja, heart failure/ja, peripheral arterial disease/ja, vision loss/ja, chronic kidney disease/ja, dementia/ja |
| Causes | 通常はライフスタイルと遺伝的要因である。 |
| Risk factors | 睡眠不足, 過剰な塩分, 過剰な体重, 喫煙, アルコール, 大気汚染 |
| Diagnostic method | 安静時の血圧 130/80 あるいは 140/90 mmHg |
| Treatment | 生活習慣の改善、薬物療法 |
| Frequency | 16–37% globally |
| Deaths | 9.4 million / 18% (2010) |
高血圧は、動脈の血圧が持続的に上昇する長期的な医学的状態である。高血圧は通常、症状を引き起こさない。しかし、脳卒中、冠動脈疾患、心不全、心房細動、末梢動脈疾患、視力低下、慢性腎臓病、認知症の主要な危険因子である。高血圧は世界中で早死にの主な原因となっている。
高血圧は一次性(本態性)高血圧と二次性高血圧に分類される。症例の約90~95%は一次性で、非特異的な生活習慣や遺伝要因による高血圧と定義される。リスクを高める生活習慣要因としては、食事中の塩分過多、過体重、喫煙、運動不足、アルコール使用が挙げられる。残りの5~10%の症例は二次性高血圧に分類され、慢性腎臓病、腎動脈の狭窄、内分泌疾患、避妊薬の使用など、明確に特定できる原因による高血圧と定義される。
血圧は2つの測定値、収縮期(高い測定値)と拡張期(低い測定値)によって分類される。ほとんどの成人にとって、安静時の正常血圧は収縮期100~130ミリメートル水銀(mmHg)および拡張期60~80mmHgの範囲内である。ほとんどの成人では、安静時血圧が130/80または140/90mmHg以上が持続する場合に高血圧となる。小児には異なる数値が適用される。24時間にわたる外来血圧測定は、診察室での血圧測定よりも正確であるように思われる。高血圧は糖尿病患者に約2倍多くみられる。
生活習慣の改善と薬物療法は血圧を下げ、健康合併症のリスクを低下させる。生活習慣の改善には、減量、身体運動、塩分摂取量の減少、アルコール摂取量の減少、健康的な食事などがある。生活様式の変更が十分でない場合は、血圧治療薬が使用される。最大3種類の薬を同時に服用することで、90%の人の血圧をコントロールすることができる。薬物による中等度の高動脈血圧(160/100mmHg以上と定義)の治療は、life expectancy/ja¥生命予後の改善と関連している。130/80 mmHgから160/100 mmHgの間の血圧に対する治療の効果はあまり明らかでなく、有益であるとするレビューもあれば、有益性は不明であるとするレビューもある。高血圧は、世界人口の16〜37%が罹患している。2010年には、高血圧が全死亡の17.8%(世界で940万人)の要因であったと考えられている。

徴候と症状
高血圧が症状を伴うことはまれであり、その同定は通常、健康スクリーニングを通して、あるいは無関係な問題のために医療を求めるときに行われる。高血圧の人の中には、頭痛(特に後頭部と午前中)のほか、ふらつき、めまい、耳鳴り(ブーンまたはヒューヒューという耳鳴り)、変視症または失神エピソードを訴える人もいる。しかし、これらの症状は、高血圧そのものではなく、関連する不安に関連している可能性がある。
身体検査では、高血圧は検眼鏡検査でみられる眼底の変化の存在と関連していることがある。高血圧性網膜症に典型的な変化の重症度はI~IVに分類され、I度およびII度の鑑別は困難である。網膜症の重症度は、高血圧の罹病期間または重症度とほぼ相関する。
二次性高血圧
二次性高血圧は、同定可能な原因による高血圧であり、特定の徴候および症状が追加されることがある。例えば、クッシング症候群は、高血圧を引き起こすだけでなく、しばしば三頭筋肥満、耐糖能異常、ムーンフェイス、首や肩の後ろの脂肪のこぶ(バッファローコンプと呼ばれる)、および紫色の腹部の妊娠線を引き起こす。甲状腺機能亢進症は食欲亢進を伴う体重減少、速い心拍数、眼球膨張、振戦を頻繁に引き起こす。腎動脈狭窄症(RAS)は、正中線の左側または右側に限局した腹部拍動を伴う(片側性RAS)こともあれば、両方の部位に伴う(両側性RAS)こともある。大動脈瘤は、腕に対する下肢の血圧低下、または大腿動脈脈拍の遅延または欠如を頻繁に引き起こす。褐色細胞腫は、頭痛、動悸、青白い外観、およびexcessive sweating/ja|過度の発汗を伴う高血圧の突然のエピソードを引き起こすことがある。
高血圧危機
重度の血圧上昇(収縮期180または拡張期120以上)を高血圧クリーゼと呼ぶ。高血圧クリーゼは、末端臓器障害の有無によって、それぞれ高血圧緊急症と高血圧緊急症に分類される。
高血圧性緊急症では、血圧上昇に起因する末端臓器障害の証拠はない。このような場合は、24~48時間かけて徐々に血圧を下げる経口薬が使用される。
高血圧性救急疾患では、1つ以上の臓器に直接的な障害が認められる。最も影響を受ける臓器には、脳、腎臓、心臓、肺があり、錯乱、眠気、胸痛、息苦しさなどの症状が現れる。高血圧緊急症では、進行中の臓器損傷を食い止めるために血圧をより急速に下げなければならないが、このアプローチに関するランダム化比較試験のエビデンスは不足している。
妊娠
高血圧は妊娠の約8~10%にみられる。6時間間隔で2回の血圧測定で140/90 mmHgを超えると、妊娠高血圧症候群と診断される。妊娠中の高血圧は、既存の高血圧、妊娠高血圧症候群、または子癇前症に分類することができる。妊娠前から慢性的な高血圧がある女性は、早産、低出生体重児、死産などの合併症のリスクが高くなる。高血圧で妊娠中に合併症があった女性は、血圧が正常で妊娠中に合併症がなかった女性と比較して、心血管疾患を発症するリスクが3倍になる。
子癇前症は、血圧上昇と尿中蛋白の存在を特徴とする、妊娠後期と分娩後の重篤な状態である。妊娠の約5%に発症し、全世界の妊産婦死亡の約16%の原因となっている。子癇前症はまた、出産前後の赤ちゃんの死亡のリスクを2倍にする。通常、子癇前症には症状がなく、定期的なスクリーニングによって発見される。子癇前症の症状が現れる場合、最も一般的なものは頭痛、視覚障害(しばしば「閃光」)、嘔吐、胃の上の痛み、むくみである。子癇前症は時に子癇と呼ばれる生命を脅かす状態に進行することがあり、これは高血圧緊急症であり、視力低下、脳腫脹、痙攣、腎不全、肺水腫、播種性血管内凝固障害(血液凝固障害)などの重篤な合併症を伴う。
一方、妊娠高血圧症候群は、尿蛋白を伴わない妊娠中の新規発症高血圧と定義される。
子どもたち
新生児や幼い乳児では、発育不全、痙攣、過敏性、元気がない、呼吸困難が高血圧と関連することがある。年長の乳児および小児では、高血圧は頭痛、原因不明の易刺激性、fatigue、発育不全、かすみ目、鼻出血、および顔面神経麻痺を引き起こすことがある。
原因
一次性高血圧
高血圧は遺伝子と環境因子の複雑な相互作用から生じる。血圧に小さな影響を及ぼす多数の一般的な遺伝的変異が同定されており、血圧に大きな影響を及ぼすいくつかのまれな遺伝的変異も同定されている。また,ゲノムワイド関連研究(GWAS)では,血圧に関連する35の遺伝子座が同定されている。同定された各新規遺伝子座のセンチネルSNPは,近傍の複数のCpG部位におけるDNAメチル化との関連を示している。これらのセンチネルSNPは、血管平滑筋と腎機能に関連する遺伝子内に位置している。DNAメチル化は,これらの関連性の根底にあるメカニズムが解明されていないにもかかわらず,共通の遺伝的変異を複数の表現型に結びつける何らかの影響を及ぼす可能性がある。本研究で行われた35のセンチネルSNP(既知および新規)に対する単一変異型検定では、遺伝的変異が単独または集合して高血圧に関連する臨床表現型のリスクに寄与することが示された。
冠動脈外反症:冠動脈外反症(CAE)は、冠動脈が他の非外反部位の1.5倍以上に拡大することを特徴とする。高血圧(HTN)患者におけるCAEのプールされた未調整のORは、HTNのない患者と比較して1.44と推定された。
血圧は、西洋型食生活やライフスタイルと関連すると加齢とともに上昇し、晩年に高血圧になるリスクは大きい。いくつかの環境因子が血圧に影響する。食塩の大量摂取は食塩に敏感な人の血圧を上昇させる;運動不足や中心性肥満は個々の症例で役割を果たすことがある。カフェインの摂取やビタミンDの欠乏などの他の因子の役割の可能性はあまり明らかではない。シンドロームX(またはメタボリックシンドローム)の構成要素であるインスリン抵抗性も高血圧の一因である。
低出生体重児,母親の喫煙,母乳育児の欠如といった幼児期の出来事は,成人本態性高血圧の危険因子である可能性があるが,これらの曝露と成人高血圧を結びつける機序は依然として不明である。未治療の高血圧患者では、正常血圧の人に比べて高血中尿酸の割合が高いことが判明しているが、前者が因果関係にあるのか、腎機能の低下に伴うものなのかは不明である。平均血圧は夏よりも冬の方が高いかもしれない。Periodontal disease/ja歯周病も高血圧と関連している。
二次性高血圧
二次性高血圧は、特定可能な原因によって生じる。腎臓病は、高血圧の最も一般的な二次的原因である。高血圧は、クッシング症候群、甲状腺機能亢進症、甲状腺機能低下症、先端巨大症、 コン症候群または高アルドステロン症、腎動脈狭窄症(アテローム性動脈硬化症または線維筋異形成による)、副甲状腺機能亢進症、および褐色細胞腫などの内分泌疾患によっても起こりうる。二次性高血圧の他の原因としては、肥満、睡眠時無呼吸症候群、妊娠、大動脈コーカクテーション、甘草の食べ過ぎ、アルコールの飲み過ぎ、特定の処方薬、漢方薬、コーヒー、コカイン、覚醒剤などの刺激物などがある。飲料水によるヒ素曝露は血圧上昇と相関することが示されている。うつ病も高血圧と関連していた。孤独も危険因子である。
2018年のレビューによると、男性ではどんなアルコールでも血圧を上昇させるが、女性では1、2杯以上の飲酒でリスクが上昇することがわかった。
病態生理学
確立された本態性高血圧のほとんどの人では、心拍出量は正常のままであるが、血流に対する抵抗の増加(全末梢抵抗)が高血圧の原因となっている。高血圧前症または'境界型高血圧'の若年者の中には、心拍出量が高く、心拍数が上昇し、末梢抵抗が正常な人がおり、運動亢進型境界型高血圧と呼ばれている。このような人は、加齢とともに心拍出量が低下し、末梢抵抗が上昇するため、後年、確立した本態性高血圧の典型的な特徴を呈するようになる。このパターンが最終的に高血圧を発症するすべての人の典型的なパターンであるかどうかは議論のあるところである。確立した高血圧における末梢抵抗の増加は、毛細血管の数や密度の減少も寄与しているかもしれないが、主に小動脈や細動脈の構造的狭窄に起因している。
動脈管の血管収縮が高血圧に関与しているかどうかは明らかではない。高血圧は末梢の静脈コンプライアンスの低下とも関連しており、静脈還流を増加させ、心臓の前負荷を増加させ、最終的には拡張機能障害を引き起こす可能性がある。
脈圧(収縮期血圧と拡張期血圧の差)は、高血圧の高齢者ではしばしば上昇する。これは収縮期血圧が異常に高く、拡張期血圧が正常または低いことを意味し、孤立性収縮期高血圧と呼ばれる状態である。高血圧または孤立性収縮期高血圧の高齢者における高い脈圧は、一般的に加齢に伴い、高血圧によって悪化する可能性のある動脈硬化の増加によって説明される。
Many mechanisms have been proposed to account for the rise in peripheral resistance in hypertension. Most evidence implicates either disturbances in the kidneys' salt and water handling (particularly abnormalities in the intrarenal renin–angiotensin system) or abnormalities of the sympathetic nervous system. These mechanisms are not mutually exclusive and it is likely that both contribute to some extent in most cases of essential hypertension. It has also been suggested that endothelial dysfunction and vascular inflammation may also contribute to increased peripheral resistance and vascular damage in hypertension. Interleukin 17 has garnered interest for its role in increasing the production of several other immune system chemical signals thought to be involved in hypertension such as tumor necrosis factor alpha, interleukin 1, interleukin 6, and interleukin 8.
Excessive sodium or insufficient potassium in the diet leads to excessive intracellular sodium, which contracts vascular smooth muscle, restricting blood flow and so increases blood pressure.
Diagnosis
Hypertension is diagnosed on the basis of a persistently high resting blood pressure. The American Heart Association (AHA) recommends at least three resting measurements on at least two separate health care visits.
In Britain, 'Blood Pressure UK' states that a healthy blood pressure is any reading between 90/60mmHg and 120/80mmHg.
Measurement technique
For an accurate diagnosis of hypertension to be made, it is essential for proper blood pressure measurement technique to be used. Improper measurement of blood pressure is common and can change the blood pressure reading by up to 10 mmHg, which can lead to misdiagnosis and misclassification of hypertension. Correct blood pressure measurement technique involves several steps. Proper blood pressure measurement requires the person whose blood pressure is being measured to sit quietly for at least five minutes which is then followed by application of a properly fitted blood pressure cuff to a bare upper arm. The person should be seated with their back supported, feet flat on the floor, and with their legs uncrossed. The person whose blood pressure is being measured should avoid talking or moving during this process. The arm being measured should be supported on a flat surface at the level of the heart. Blood pressure measurement should be done in a quiet room so the medical professional checking the blood pressure can hear the Korotkoff sounds while listening to the brachial artery with a stethoscope for accurate blood pressure measurements. The blood pressure cuff should be deflated slowly (2–3 mmHg per second) while listening for the Korotkoff sounds. The bladder should be emptied before a person's blood pressure is measured since this can increase blood pressure by up to 15/10 mmHg. Multiple blood pressure readings (at least two) spaced 1–2 minutes apart should be obtained to ensure accuracy. Ambulatory blood pressure monitoring over 12 to 24 hours is the most accurate method to confirm the diagnosis. An exception to this is those with very high blood pressure readings especially when there is poor organ function.
With the availability of 24-hour ambulatory blood pressure monitors and home blood pressure machines, the importance of not wrongly diagnosing those who have white coat hypertension has led to a change in protocols. In the United Kingdom, current best practice is to follow up a single raised clinic reading with ambulatory measurement, or less ideally with home blood pressure monitoring over the course of 7 days. The United States Preventive Services Task Force also recommends getting measurements outside of the healthcare environment. Pseudohypertension in the elderly or noncompressibility artery syndrome may also require consideration. This condition is believed to be due to calcification of the arteries resulting in abnormally high blood pressure readings with a blood pressure cuff while intra arterial measurements of blood pressure are normal. Orthostatic hypertension is when blood pressure increases upon standing.
Other investigations
| System | Tests |
|---|---|
| Kidney | Microscopic urinalysis, protein in the urine, BUN, creatinine |
| Endocrine | Serum sodium, potassium, calcium, TSH |
| Metabolic | Fasting blood glucose, HDL, LDL, total cholesterol, triglycerides |
| Other | Hematocrit, electrocardiogram, chest radiograph |
Once the diagnosis of hypertension has been made, healthcare providers should attempt to identify the underlying cause based on risk factors and other symptoms, if present. Secondary hypertension is more common in preadolescent children, with most cases caused by kidney disease. Primary or essential hypertension is more common in adolescents and adults and has multiple risk factors, including obesity and a family history of hypertension. Laboratory tests can also be performed to identify possible causes of secondary hypertension, and to determine whether hypertension has caused damage to the heart, eyes, and kidneys. Additional tests for diabetes and high cholesterol levels are usually performed because these conditions are additional risk factors for the development of heart disease and may require treatment.
Initial assessment of the hypertensive people should include a complete history and physical examination. Serum creatinine is measured to assess for the presence of kidney disease, which can be either the cause or the result of hypertension. Serum creatinine alone may overestimate glomerular filtration rate and the 2003 JNC7 guidelines advocate the use of predictive equations such as the Modification of Diet in Renal Disease (MDRD) formula to estimate glomerular filtration rate (eGFR). eGFR can also provide a baseline measurement of kidney function that can be used to monitor for side effects of certain anti-hypertensive drugs on kidney function. Additionally, testing of urine samples for protein is used as a secondary indicator of kidney disease. Electrocardiogram (EKG/ECG) testing is done to check for evidence that the heart is under strain from high blood pressure. It may also show whether there is thickening of the heart muscle (left ventricular hypertrophy) or whether the heart has experienced a prior minor disturbance such as a silent heart attack. A chest X-ray or an echocardiogram may also be performed to look for signs of heart enlargement or damage to the heart.
Classification in adults
| Categories | Systolic blood pressure, mmHg | And/or | Diastolic blood pressure, mmHg | ||
|---|---|---|---|---|---|
| Method | Office | 24h ambulatory | Office | 24h ambulatory | |
| Hypotension | <110 | <100 | or | <70 | <60 |
| American College of Cardiology/American Heart Association (2017) | |||||
| Normal | <120 | <115 | and | <80 | <75 |
| Elevated | 120–129 | 115–124 | and | <80 | <75 |
| Hypertension, stage 1 | 130–139 | 125–129 | or | 80–89 | 75–79 |
| Hypertension, stage 2 | ≥140 | ≥130 | or | ≥90 | ≥80 |
| European Society of Hypertension (2023) | |||||
| Optimal | <120 | — | and | <80 | — |
| Normal | 120–129 | — | and/or | 80–84 | — |
| High normal | 130–139 | — | and/or | 85–89 | — |
| Hypertension, grade 1 | 140–159 | ≥130 | and/or | 90–99 | ≥80 |
| Hypertension, grade 2 | 160–179 | — | and/or | 100–109 | — |
| Hypertension, grade 3 | ≥180 | — | and/or | ≥110 | — |
In people aged 18 years or older, hypertension is defined as either a systolic or a diastolic blood pressure measurement consistently higher than an accepted normal value (this is above 129 or 139 mmHg systolic, 89 mmHg diastolic depending on the guideline). Lower thresholds are used if measurements are derived from 24-hour ambulatory or home monitoring.
Children
Hypertension occurs in around 0.2 to 3% of newborns; however, blood pressure is not measured routinely in healthy newborns. Hypertension is more common in high risk newborns. A variety of factors, such as gestational age, postconceptional age and birth weight needs to be taken into account when deciding if a blood pressure is normal in a newborn.
Hypertension defined as elevated blood pressure over several visits affects 1% to 5% of children and adolescents and is associated with long-term risks of ill-health. Blood pressure rises with age in childhood and, in children, hypertension is defined as an average systolic or diastolic blood pressure on three or more occasions equal or higher than the 95th percentile appropriate for the sex, age and height of the child. High blood pressure must be confirmed on repeated visits however before characterizing a child as having hypertension. Prehypertension in children has been defined as average systolic or diastolic blood pressure that is greater than or equal to the 90th percentile, but less than the 95th percentile. In adolescents, it has been proposed that hypertension and pre-hypertension are diagnosed and classified using the same criteria as in adults.
High blood pressure is frequently encountered in pediatric emergency and outpatient clinics, one of the simplest and reliable methods to assess the need for referral and or further action is the score developed by Elbaba M., published in 2018. The score is composed of a set of 10 items with grades 1, 2 or 3 for each item. The author assumed the mid score of 15 or less is not associated with true hypertension, it can be reactive, white-coat or unreliable measurement. And the score of 16 or above reflects a warning alarm to true hypertension that usually require monitoring, investigations and or treatment.
Prevention
Much of the disease burden of high blood pressure is experienced by people who are not labeled as hypertensive. Consequently, population strategies are required to reduce the consequences of high blood pressure and reduce the need for antihypertensive medications. Lifestyle changes are recommended to lower blood pressure, before starting medications. The 2004 British Hypertension Society guidelines proposed lifestyle changes consistent with those outlined by the US National High BP Education Program in 2002 for the primary prevention of hypertension:
- maintain normal body weight for adults (e.g. body mass index 20–25 kg/m2)
- reduce dietary sodium intake to <100 mmol/ day (<6 g of sodium chloride or <2.4 g of sodium per day)
- engage in regular aerobic physical activity such as brisk walking (≥30 min per day, most days of the week)
- limit alcohol consumption to no more than 3 units/day in men and no more than 2 units/day in women
- consume a diet rich in fruit and vegetables (e.g. at least five portions per day);
- stress reduction
Avoiding or learning to manage stress can help a person control blood pressure.
A few relaxation techniques that can help relieve stress are:
- meditation
- warm baths
- yoga
- going on long walks
Effective lifestyle modification may lower blood pressure as much as an individual antihypertensive medication. Combinations of two or more lifestyle modifications can achieve even better results. There is considerable evidence that reducing dietary salt intake lowers blood pressure, but whether this translates into a reduction in mortality and cardiovascular disease remains uncertain. Estimated sodium intake ≥6g/day and <3g/day are both associated with high risk of death or major cardiovascular disease, but the association between high sodium intake and adverse outcomes is only observed in people with hypertension. Consequently, in the absence of results from randomized controlled trials, the wisdom of reducing levels of dietary salt intake below 3g/day has been questioned. ESC guidelines mention periodontitis is associated with poor cardiovascular health status.
The value of routine screening for hypertension is debated. In 2004, the National High Blood Pressure Education Program recommended that children aged 3 years and older have blood pressure measurement at least once at every health care visit and the National Heart, Lung, and Blood Institute and American Academy of Pediatrics made a similar recommendation. However, the American Academy of Family Physicians supports the view of the U.S. Preventive Services Task Force that the available evidence is insufficient to determine the balance of benefits and harms of screening for hypertension in children and adolescents who do not have symptoms. The US Preventive Services Task Force recommends screening adults 18 years or older for hypertension with office blood pressure measurement.
Management
According to one review published in 2003, reduction of the blood pressure by 5 mmHg can decrease the risk of stroke by 34%, of ischemic heart disease by 21%, and reduce the likelihood of dementia, heart failure, and mortality from cardiovascular disease.
Target blood pressure
Various expert groups have produced guidelines regarding how low the blood pressure target should be when a person is treated for hypertension. These groups recommend a target below the range 140–160 / 90–100 mmHg for the general population. Cochrane reviews recommend similar targets for subgroups such as people with diabetes and people with prior cardiovascular disease. Additionally, Cochrane reviews have found that for older individuals with moderate to high cardiovascular risk, the benefits of trying to achieve a lower than standard blood pressure target (at or below 140/90 mmHg) are outweighed by the risk associated with the intervention. These findings may not be applicable to other populations.
Many expert groups recommend a slightly higher target of 150/90 mmHg for those over somewhere between 60 and 80 years of age. The JNC-8 and American College of Physicians recommend the target of 150/90 mmHg for those over 60 years of age, but some experts within these groups disagree with this recommendation. Some expert groups have also recommended slightly lower targets in those with diabetes or chronic kidney disease with protein loss in the urine, but others recommend the same target as for the general population. The issue of what is the best target and whether targets should differ for high risk individuals is unresolved, although some experts propose more intensive blood pressure lowering than advocated in some guidelines.
For people who have never experienced cardiovascular disease who are at a 10-year risk of cardiovascular disease of less than 10%, the 2017 American Heart Association guidelines recommend medications if the systolic blood pressure is >140 mmHg or if the diastolic BP is >90 mmHg. For people who have experienced cardiovascular disease or those who are at a 10-year risk of cardiovascular disease of greater than 10%, it recommends medications if the systolic blood pressure is >130 mmHg or if the diastolic BP is >80 mmHg.
Lifestyle modifications
The first line of treatment for hypertension is lifestyle changes, including dietary changes, physical activity, and weight loss. Though these have all been recommended in scientific advisories, a Cochrane systematic review found no evidence (due to lack of data) for effects of weight loss diets on death, long-term complications or adverse events in persons with hypertension. The review did find a decrease in body weight and blood pressure. Their potential effectiveness is similar to and at times exceeds a single medication. If hypertension is high enough to justify immediate use of medications, lifestyle changes are still recommended in conjunction with medication.
Dietary changes shown to reduce blood pressure include diets with low sodium, the DASH diet (Dietary Approaches to Stop Hypertension), which was the best against 11 other diet in an umbrella review, and plant-based diets. There is some evidence green tea consumption may help lower blood pressure, but this is insufficient for it to be recommended as a treatment. There is evidence from randomized, double-blind, placebo-controlled clinical trials that Hibiscus tea consumption significantly reduces systolic blood pressure (-4.71 mmHg, 95% CI [-7.87, -1.55]) and diastolic blood pressure (−4.08 mmHg, 95% CI [-6.48, −1.67]). Beetroot juice consumption also significantly lowers the blood pressure of people with high blood pressure.
Increasing dietary potassium has a potential benefit for lowering the risk of hypertension. The 2015 Dietary Guidelines Advisory Committee (DGAC) stated that potassium is one of the shortfall nutrients which is under-consumed in the United States. However, people who take certain antihypertensive medications (such as ACE-inhibitors or ARBs) should not take potassium supplements or potassium-enriched salts due to the risk of high levels of potassium.
Physical exercise regimens which are shown to reduce blood pressure include isometric resistance exercise, aerobic exercise, resistance exercise, and device-guided breathing.
Stress reduction techniques such as biofeedback or transcendental meditation may be considered as an add-on to other treatments to reduce hypertension, but do not have evidence for preventing cardiovascular disease on their own. Self-monitoring and appointment reminders might support the use of other strategies to improve blood pressure control, but need further evaluation.
Medications
Several classes of medications, collectively referred to as antihypertensive medications, are available for treating hypertension.
First-line medications for hypertension include thiazide-diuretics, calcium channel blockers, angiotensin converting enzyme inhibitors (ACE inhibitors), and angiotensin receptor blockers (ARBs). These medications may be used alone or in combination (ACE inhibitors and ARBs are not recommended for use together); the latter option may serve to minimize counter-regulatory mechanisms that act to restore blood pressure values to pre-treatment levels, although the evidence for first-line combination therapy is not strong enough. Most people require more than one medication to control their hypertension. Medications for blood pressure control should be implemented by a stepped care approach when target levels are not reached. Withdrawal of such medications in the elderly can be considered by healthcare professionals, because there is no strong evidence of an effect on mortality, myocardial infarction, or stroke.
Previously, beta-blockers such as atenolol were thought to have similar beneficial effects when used as first-line therapy for hypertension. However, a Cochrane review that included 13 trials found that the effects of beta-blockers are inferior to that of other antihypertensive medications in preventing cardiovascular disease.
The prescription of antihypertensive medication for children with hypertension has limited evidence. There is limited evidence which compare it with placebo and shows modest effect to blood pressure in short term. Administration of higher dose did not make the reduction of blood pressure greater.
Resistant hypertension
Resistant hypertension is defined as high blood pressure that remains above a target level, in spite of being prescribed three or more antihypertensive drugs simultaneously with different mechanisms of action. Failing to take prescribed medications as directed is an important cause of resistant hypertension. Resistant hypertension may also result from chronically high activity of the autonomic nervous system, an effect known as neurogenic hypertension. Electrical therapies that stimulate the baroreflex are being studied as an option for lowering blood pressure in people in this situation.
Some common secondary causes of resistant hypertension include obstructive sleep apnea, pheochromocytoma, renal artery stenosis, coarctation of the aorta, and primary aldosteronism. As many as one in five people with resistant hypertension have primary aldosteronism, which is a treatable and sometimes curable condition.
Refractory hypertension
Refractory hypertension is characterized by uncontrolled elevated blood pressure unmitigated by five or more antihypertensive agents of different classes, including a long-acting thiazide-like diuretic, a calcium channel blocker, and a blocker of the renin-angiotensin system. People with refractory hypertension typically have increased sympathetic nervous system activity, and are at high risk for more severe cardiovascular diseases and all-cause mortality.
Non-modulating
Non-modulating essential hypertension is a form of salt-sensitive hypertension, where sodium intake does not modulate either adrenal or renal vascular responses to angiotensin II. Individuals with this subset have been termed non-modulators. They make up 25–30% of the hypertensive population.
Epidemiology
| no data <110 110–220 220–330 330–440 440–550 550–660 | 660–770 770–880 880–990 990–1100 1100–1600 >1600 |
Adults
2019年現在[update], at least 1 billion 278 million adults aged 30–79 worldwide (over 16% of world population), including 626 million women and 652 million men, were estimated to have hypertension. This is approximately 278 million up from 2014 and almost double compared to year 1990, when there were estimated 648 million adults in the same age group living with the condition worldwide.
Hypertension is slightly more frequent in men, in those of low socioeconomic status, and it becomes more common with age. It is common in high, medium, and low-income countries. In 2004, rates of high blood pressure were highest in Africa (30% for both sexes), and lowest in the Americas (18% for both sexes). Rates also vary markedly within regions with country-level rates as low as 22.8% (men) and 18.4% (women) in Peru and as high as 61.6% (men) and 50.9% (women) in Paraguay. Rates in Africa were about 45% in 2016.
In Europe, hypertension occurs in about 30–45% of people 2013年現在[update]. In 1995 it was estimated that 43 million people (24% of the population) in the United States had hypertension or were taking antihypertensive medication. By 2004 this had increased to 29% and further to 32% (76 million US adults) by 2017. In 2017, with the change in definitions for hypertension, 46% of people in the United States are affected. African-American adults in the United States have among the highest rates of hypertension in the world at 44%. It is also more common in Filipino Americans and less common in US whites and Mexican Americans. Differences in hypertension rates are multifactorial and under study.
Children
Rates of high blood pressure in children and adolescents have increased in the last 20 years in the United States. Childhood hypertension, particularly in pre-adolescents, is more often secondary to an underlying disorder than in adults. Kidney disease is the most common secondary cause of hypertension in children and adolescents. Nevertheless, primary or essential hypertension accounts for most cases.
Prognosis
Hypertension is the most important preventable risk factor for premature death worldwide. It increases the risk of ischemic heart disease, strokes, peripheral vascular disease, and other cardiovascular diseases, including heart failure, aortic aneurysms, diffuse atherosclerosis, chronic kidney disease, atrial fibrillation, cancers, leukemia and pulmonary embolism. Hypertension is also a risk factor for cognitive impairment and dementia. Other complications include hypertensive retinopathy and hypertensive nephropathy.
History
Measurement
Modern understanding of the cardiovascular system began with the work of physician William Harvey (1578–1657), who described the circulation of blood in his book "De motu cordis". The English clergyman Stephen Hales made the first published measurement of blood pressure in 1733. However, hypertension as a clinical entity came into its own with the invention of the cuff-based sphygmomanometer by Scipione Riva-Rocci in 1896. This allowed easy measurement of systolic pressure in the clinic. In 1905, Nikolai Korotkoff improved the technique by describing the Korotkoff sounds that are heard when the artery is ausculted with a stethoscope while the sphygmomanometer cuff is deflated. This permitted systolic and diastolic pressure to be measured.
Identification
The symptoms similar to symptoms of patients with hypertensive crisis are discussed in medieval Persian medical texts in the chapter of "fullness disease". The symptoms include headache, heaviness in the head, sluggish movements, general redness and warm to touch feel of the body, prominent, distended and tense vessels, fullness of the pulse, distension of the skin, coloured and dense urine, loss of appetite, weak eyesight, impairment of thinking, yawning, drowsiness, vascular rupture, and hemorrhagic stroke. Fullness disease was presumed to be due to an excessive amount of blood within the blood vessels.
Descriptions of hypertension as a disease came among others from Thomas Young in 1808 and especially Richard Bright in 1836. The first report of elevated blood pressure in a person without evidence of kidney disease was made by Frederick Akbar Mahomed (1849–1884).
Until the 1990s, systolic hypertension was defined as systolic blood pressure of 160 mm Hg or greater. In 1993, the WHO/ISH guidelines defined 140 mmHg as the threshold for hypertension.
Treatment
Historically the treatment for what was called the "hard pulse disease" consisted in reducing the quantity of blood by bloodletting or the application of leeches. This was advocated by The Yellow Emperor of China, Cornelius Celsus, Galen, and Hippocrates. The therapeutic approach for the treatment of hard pulse disease included changes in lifestyle (staying away from anger and sexual intercourse) and dietary program for patients (avoiding the consumption of wine, meat, and pastries, reducing the volume of food in a meal, maintaining a low-energy diet and the dietary usage of spinach and vinegar).
In the 19th and 20th centuries, before effective pharmacological treatment for hypertension became possible, three treatment modalities were used, all with numerous side-effects: strict sodium restriction (for example the rice diet), sympathectomy (surgical ablation of parts of the sympathetic nervous system), and pyrogen therapy (injection of substances that caused a fever, indirectly reducing blood pressure).
The first chemical for hypertension, sodium thiocyanate, was used in 1900 but had many side effects and was unpopular. Several other agents were developed after the Second World War, the most popular and reasonably effective of which were tetramethylammonium chloride, hexamethonium, hydralazine, and reserpine (derived from the medicinal plant Rauvolfia serpentina). None of these were well tolerated. A major breakthrough was achieved with the discovery of the first well-tolerated orally available agents. The first was chlorothiazide, the first thiazide diuretic and developed from the antibiotic sulfanilamide, which became available in 1958. Subsequently, beta blockers, calcium channel blockers, angiotensin converting enzyme (ACE) inhibitors, angiotensin receptor blockers, and renin inhibitors were developed as antihypertensive agents.
社会と文化
意識
世界保健機関は、高血圧を心血管系死亡率の主要な原因としている。世界高血圧連盟(WHL)は、85カ国の高血圧学会と高血圧連盟の統括組織であるが、世界の高血圧人口の50%以上が自分の状態に気づいていないことを認識していた。この問題に取り組むため、WHLは2005年に高血圧に関する世界的な啓発キャンペーンを開始し、毎年5月17日を世界高血圧デー(WHD)と定めた。過去3年間で、より多くの国の学会がWHDに参加し、一般の人々にメッセージを伝えるために革新的な活動を行ってきた。2007年には、WHLの47の加盟国から記録的な参加があった。WHDの一週間、これらの国々は、それぞれの地方自治体、専門家協会、非政府組織、民間産業と連携して、いくつかのメディアや市民集会を通じて、国民の間に高血圧の認識を広めた。インターネットやテレビなどのマスメディアを利用して、そのメッセージは2億5,000万人以上に届いた。この勢いは年々加速しており、WHLは、高血圧に罹患していると推定される15億人のほぼ全員にメッセージを届けることができると確信している。
経済学
高血圧は、アメリカの初期医療機関を訪れる際の最も一般的な慢性医療問題である。アメリカ心臓協会によると、2010年の高血圧の直接および間接的なコストは766億ドルと推定されている。アメリカでは、高血圧の患者のうち80%がその状態を認識しており、71%が抗高血圧薬を服用しているが、高血圧であることを認識している人のうち48%しか適切にコントロールしていない。高血圧の適切な管理は、高血圧の診断、治療、またはコントロールにおける不足によって妨げられることがある。 Health care providers/ja医療提供者 は、複数の薬を服用して血圧目標を達成する抵抗感など、血圧コントロールを達成するために多くの障害に直面している。また、人々は薬のスケジュールを守ることやライフスタイルの変更に対処することにも困難を感じている。それでも、血圧目標の達成は可能であり、最も重要なことは、血圧を有意に下げることが心臓病や脳卒中による死亡リスク、他の機能障害の発症、高度な医療ケアに伴う費用を大幅に減少させることある。
その他の動物
猫の高血圧は収縮期血圧が150 mmHg以上で適応となり、アムロジピンが通常の第一選択薬となる。収縮期血圧が170mmHgを超える猫は高血圧とみなされる。もし猫が腎臓病や網膜剥離のような他の問題を抱えているならば、160 mmHG以下の血圧もモニターする必要があるかもしれない。
犬の正常血圧は犬種によって大きく異なるが、収縮期血圧が160 mmHgを超える場合、特に標的臓器障害を伴う場合は高血圧と診断されることが多い。犬の高血圧の治療には、レニン・アンジオテンシン系の阻害薬やカルシウム拮抗薬が用いられることが多いが、高血圧を引き起こす特定の疾患に対しては他の薬剤が適応となることもある。
さらに読む
- James PA, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, Handler J, et al. (February 2014). "2014 evidence-based guideline for the management of high blood pressure in adults: report from the panel members appointed to the Eighth Joint National Committee (JNC 8)". JAMA. 311 (5): 507–20. doi:10.1001/jama.2013.284427. PMID 24352797.